What Is Bipolar Affective Disorder And How Is It Treated?

INTRODUCTION
A prolonged feeling or emotion that dominates a person’s actions and affects his or her perception is referred to as “mood”. Unipolar and bipolar disorders are examples of mood disorders, often known as affective disorders. Bipolar Affective Disorder (BPAD) is a chronic and complex mood disorder characterised by a combination of manic (bipolar mania), hypomanic (bipolar depression), and depressive (bipolar depression) episodes, as well as significant subsyndromal symptoms that commonly occur between major mood episodes. Bipolar disorder is a mental illness that produces significant mood fluctuations, including emotional highs (mania or hypomania) and lows (manic depression) (depression).
In the general population, the lifetime prevalence of BPAD I is approximately 1%. Bipolar disorder usually appears in early adulthood, between the ages of 18 and 20, while some data point to a later beginning (>25 years of age).

During the depressive phase, some patients may feel gloomy or hopeless, and lose interest or pleasure in activities. They may feel ecstatic, full of energy, or abnormally irritable as their mood switches to mania or hypomania (a milder form of mania). Sleep, energy, activity, judgement, conduct, and the ability to think clearly can all be affected by mood fluctuations. Mood swings can occur anywhere from once a year to several times a year. Some people have emotional symptoms, whereas others do not.
SYMPTOMS
Bipolar and associated diseases can manifest themselves in a variety of ways. Mania, hypomania, and depression are examples. Symptoms might induce mood and behaviour changes that are unpredictable, causing severe distress and making it difficult to operate. Bipolar disorder can strike at any age, but it is most commonly diagnosed in adolescence or early adulthood. Symptoms differ from person to person, and they can change over time. Broadly, it can be of the following types:

Bipolar I Disorder - A person may have at least one manic episode, which may or may not be preceded or followed by hypomanic or major depressive episodes. Mania can also cause a detachment from reality in some people (psychosis).
Bipolar II Disorder - Individuals may have had at least one severe depressive episode and one hypomanic episode, but never a manic episode.
Cyclothymic Disorder - The individual experienced at least a year or two of hypomania symptoms and bouts of depressive symptoms (but not as severe as major depression). Cyclothymia means recurring cycles of mood disturbances, if not treated.
COMPONENTS OF BPAD
Major Depressive Episode - A Major Depressive Episode is defined as a set of symptoms that are severe enough to interfere with daily activities such as job, school, social activities, or relationships. Five or more of the following symptoms are present during an episode:
• Sad, empty, hopeless, or sorrowful moods are all examples of depressed moods (in children and teens, depressed mood can appear as irritability)
• All or almost all activities have a noticeable lack of interest or pleasure
• When not dieting, significant weight reduction, weight gain, or a decrease or increase in appetite are all possible outcomes (in children, failure to gain weight as expected can be a sign of depression)
• Insomnia or excessive sleeping
• Fatigue or a lack of energy is a common occurrence
• Feelings of worthlessness or inappropriate or excessive guilt
• Indecisiveness or a decreased ability to ponder or concentrate
• Suicide is something that many people consider, plan, or try
Lastly, Either agitation or a slower pace.

Mania And Hypomania - Mania is more severe than hypomania, and it produces more obvious problems at job, school, and social activities, as well as relationship issues. Mania can sometimes lead to a loss of consciousness (psychosis), which may necessitate hospitalisation.
Both a manic and a hypomanic episode include three or more of these symptoms:
• A person who is abnormally enthusiastic, jumpy, or wired
• An increase in activity, energy, or agitation is a sign of increased activity, energy, or agitation
• Self-assurance and an exaggerated sense of well-being (euphoria)
• Sleeping needs are reduced.
• Unusual chattiness
• Thoughts whirling
• Distractibility
• Poor decision-making — for example, going on buying sprees, taking sexual risks or making foolish investments.
CAUSES OF BPAD
A range of variables can contribute to bipolar affective disorder. The following are a few of them:
• Genetics - People with bipolar disorder are more likely to have a first-degree family with the illness, such as a sibling or parent.
• Neuroanatomy - Emotion control, response conditioning, and behaviour reaction to stimuli are all aided by the prefrontal cortex, anterior cingulate cortex, hippocampus, and amygdala.
• Structural And Functional Imaging - In bipolar disorder, abnormal hyperintensities in subcortical regions, including the thalamus, basal ganglia, and periventricular area, signal repeated episodes and neurodegeneration have been noted. Patients with severe depression or a family history of mood disorders had higher glucose metabolism in the limbic region and lower metabolism in the frontal lobe.
• Hormone Regulation Imbalance - Mania is marked by increased adrenocortical activity. Chronic stress inhibits neurogenesis and neuroplasticity by lowering the neurokinin brain-derived neurotrophic factor (BDNF).
• Psychosocial Factors - Neuronal changes such as neurotransmitter levels, synaptic signalling abnormalities, and neuronal death may occur as a result of certain events such as a substantial life stressor or traumatic situations.
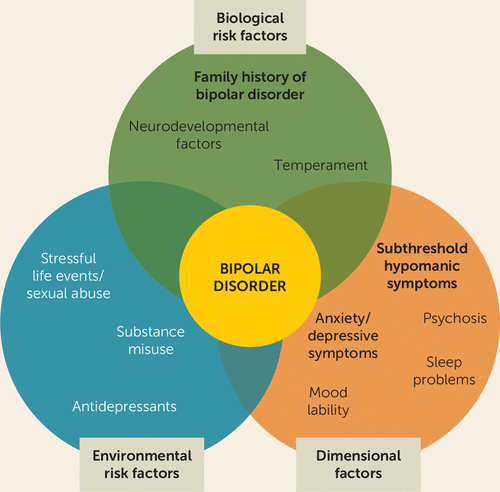
RISK FACTORS
The following are some of the things that may raise your risk of having bipolar illness or act as a trigger for your first episode:
-Having a first-degree family with bipolar disorder, such as a parent or sibling
-Stressful events, such as a loved one's death or another catastrophic incident
-Abuse of drugs or alcohol
CO-OCCURRING CONDITIONS
If you’ve been diagnosed with bipolar illness, you may also have another medical condition that requires treatment in addition to the bipolar disorder. Some disorders can exacerbate the symptoms of bipolar disorder or make treatment less effective. For example:
• Anxiety disorders
• Eating disorders
• Attention-deficit/hyperactivity disorder (ADHD)
• Alcohol or drug problems
• Physical health problems, such as heart disease, thyroid problems, headaches or obesity
SUBSEQUENT EPISODE PREVENTION
There is no one-size-fits-all approach to preventing bipolar disorder. Seeking therapy at the first sign of any mental health condition is one strategy to avoid symptoms from escalating. Minor symptoms can be prevented from becoming full-blown episodes of mania or depression by using the following strategies:
•Keep an eye out for warning signals. Getting therapy as soon as possible will help avoid bouts of bipolar affective disorder from getting worse. It’s possible that you’ve seen a pattern in your bipolar episodes and what causes them. You might also enlist the help of family members or friends to keep an eye out for warning indicators.
• Stay away from drugs and alcohol. Alcohol or recreational drugs can exacerbate your symptoms and make them more likely to return.
• Follow your doctor’s instructions for taking your medications. Withdrawal symptoms may occur if you stop taking your medicine or reduce your dose on your own, and your symptoms may worsen or return.

MANAGEMENT
The fundamental goals of pharmacological treatment for Bipolar Affective Disorder are to protect the safety of patients and those around them, as well as to achieve clinical and functional stabilisation with the fewest potential side effects. In addition, in any chronic condition requiring long-term adherence, participation in therapy and the creation of a therapeutic alliance is critical, and this collaboration is especially vital during the initial episode.

Antipsychotics and Mood Stabilisers are the cornerstones of acute bipolar mania and depression treatment. The main pharmaceutical medicines used to treat bipolar affective disorder, particularly in the maintenance period of mania, are mood stabilisers.
Cognitive behavioural therapy (CBT), interpersonal and social rhythm therapy (IPSRT), and family-focused therapy are among psychosocial treatment options for bipolar disorder.
Cognitive Behavioral Therapy: According to the American Psychological Association, incorporating cognitive-behavioral therapy to a treatment plan can enhance the result of bipolar disorder. Cognitive Behavioral therapy (CBT) entails altering one's thinking patterns as well as role plays for more successful interactions and communication.
Interpersonal and Social Rhythm Therapy (IPSRT): IPSRT is utilised with Bipolar Affective Disorder patients to improve communication, medication adherence, and stress management.
Antipsychotic or mood-stabilizing drugs may be required for the majority of people with bipolar disorder. Psychosocial therapy may be given to improve the individual’s functioning, medication adherence, developing effective coping skills, trigger protection, and trigger management in a healthier way.

